30 Oct Understanding Psoriatic Arthritis
Psoriatic arthritis is a chronic autoimmune disease that affects the joints and skin of individuals with psoriasis. It is estimated that around 30 percent of people with psoriasis will develop psoriatic arthritis at some point in their lives. In this article, we will discuss the symptoms, diagnosis, and treatment options for psoriatic arthritis, as well as how a rheumatologist like Craig Orofino from Island Rheumatology can help.
Symptoms of Psoriatic Arthritis:
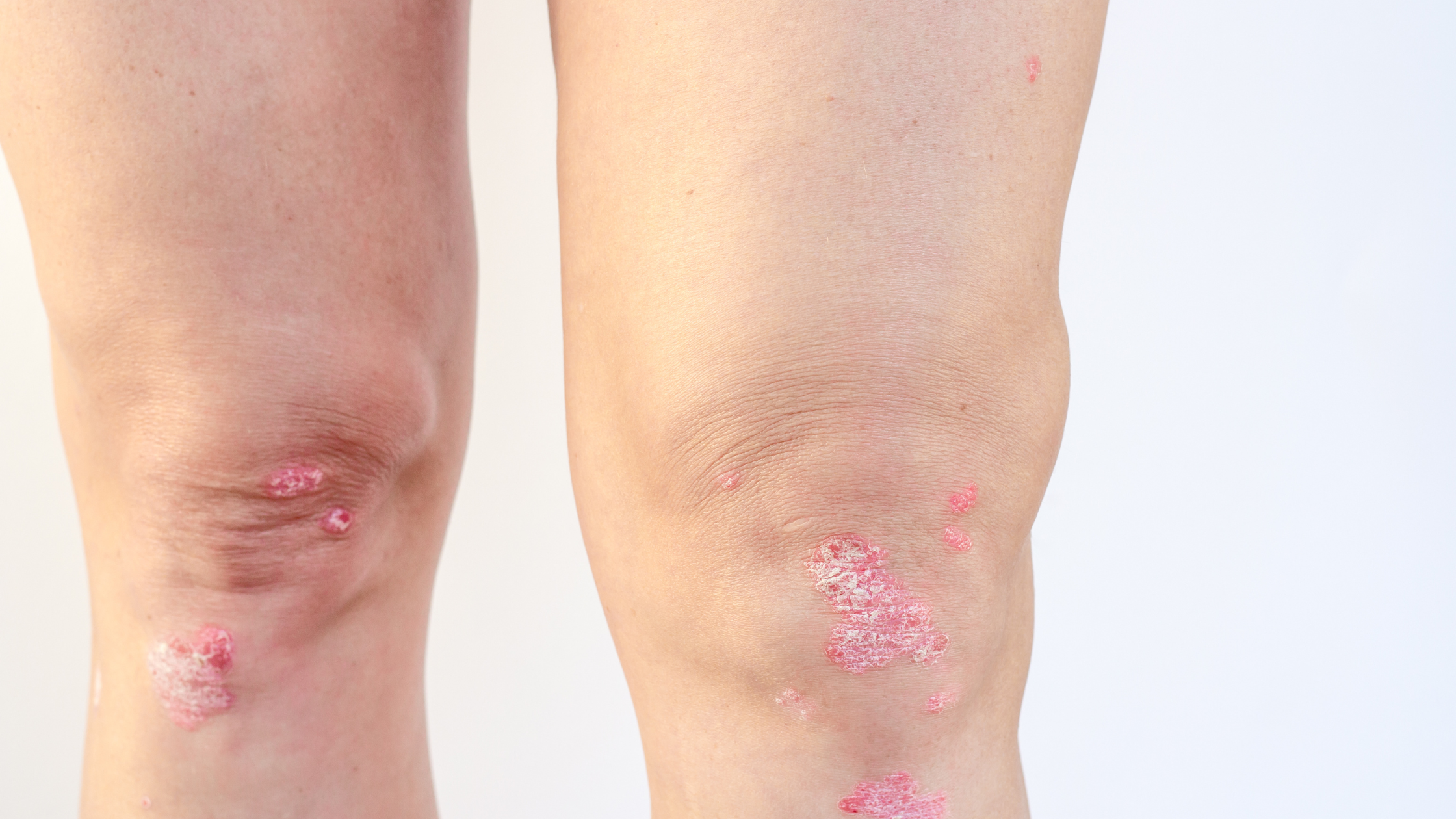
Psoriatic arthritis can cause a variety of symptoms that can vary in severity from person to person. The most common symptoms include joint pain, stiffness, and swelling, which may be especially pronounced in the morning or after periods of inactivity. The joints most commonly affected are the fingers, toes, lower back, and knees. Other symptoms may include fatigue, nail changes such as pitting or separation from the nail bed, and red or silvery scaly skin patches.
Diagnosis of Psoriatic Arthritis:
Diagnosing psoriatic arthritis can be challenging, as its symptoms can overlap with other types of arthritis. A rheumatologist will typically evaluate the patient’s medical history and perform a physical examination to assess joint symptoms and skin changes. Imaging tests such as X-rays or magnetic resonance imaging (MRI) may be used to evaluate joint damage and inflammation. However, there are no specific tests available to definitively diagnose psoriatic arthritis.
Laboratory tests can help support the diagnosis by ruling out other conditions and assessing inflammation levels. A blood test called the erythrocyte sedimentation rate (ESR) or C-reactive protein (CRP) may be elevated in individuals with psoriatic arthritis. Additionally, testing for the presence of certain antibodies, such as rheumatoid factor or anti-cyclic citrullinated peptide (anti-CCP) antibodies, can also help differentiate psoriatic arthritis from other types of arthritis. The HLA-B27 genetic marker may help in diagnosis, however it is not diagnostic.
Treatments for Psoriatic Arthritis:
The goal of treatment for psoriatic arthritis is to alleviate symptoms, prevent joint damage, and improve quality of life. Treatment plans are usually tailored to the individual’s specific needs and may involve a combination of medications, lifestyle changes, and physical therapy.
Nonsteroidal anti-inflammatory drugs (NSAIDs) are often recommended to reduce pain and inflammation. Disease-modifying antirheumatic drugs (DMARDs), such as methotrexate or sulfasalazine, can help slow down the progression of joint damage. Biologic drugs, such as
tumor necrosis factor (TNF) inhibitors or interleukin-17 (IL-17) inhibitors, may also be prescribed to target specific aspects of the immune system.
In addition to medications, lifestyle modifications can also play a crucial role in managing psoriatic arthritis. Regular exercise can help improve joint flexibility and strength, while also promoting overall well-being. Physical therapy may be recommended to learn specific exercises and techniques to manage symptoms. It is also important for individuals with psoriatic arthritis to maintain a healthy weight, as excess weight can put added stress on the joints.
How Craig Orofino, Rheumatologist, Can Help:
A rheumatologist like Craig Orofino from Island Rheumatology is a medical specialist who is trained in diagnosing and treating conditions that affect the joints, muscles, and bones. In the case of psoriatic arthritis, a rheumatologist can help by:
- Diagnosing the condition accurately: Rheumatologists have the expertise to accurately diagnose psoriatic arthritis by considering various factors, such as medical history, physical examination, and laboratory tests.
- Developing a personalized treatment plan: A rheumatologist can create an individualized treatment plan for each patient, taking into account their specific symptoms, progression of the disease, and overall health. They can recommend the most appropriate medications, lifestyle changes, and therapeutic interventions to manage the symptoms and prevent further joint damage.
- Monitoring disease progression: Psoriatic arthritis is a chronic condition that can worsen over time. A rheumatologist can monitor the disease’s progression through regular check-ups, imaging tests, and laboratory tests. They can adjust the treatment plan accordingly to ensure effective management.
- Providing education and support: Rheumatologists can help patients understand their condition better and provide them with the necessary information and resources to manage their symptoms. They can also provide emotional support and address any concerns or questions the patient may have.
In conclusion, psoriatic arthritis is a chronic autoimmune disease that affects the joints and skin of individuals with psoriasis. It can cause joint pain, stiffness, and swelling, as well as skin changes and fatigue. Diagnosis involves a combination of clinical evaluation and laboratory tests to rule out other conditions. Treatment options include medications, lifestyle changes, and physical therapy. A rheumatologist like Craig Orofino from Island Rheumatology can play a crucial role in diagnosing and managing psoriatic arthritis by providing accurate diagnosis, developing personalized treatment plans, monitoring disease progression, and providing education and support to patients.
